Imagine discovering Permanent Cure For Psoriasis might lie not just in medications or topical treatments, but in restoring your body’s internal systems! Psoriasis is a chronic autoimmune condition that impacts millions of people around the globe. It’s much more than just a skin issue; it involves a fascinating mix of immune dysfunction, hormonal imbalances, and systemic inflammation.
While traditional treatments often aim to ease symptoms, exciting new research and holistic approaches—like Hormone Reset’s functional medicine-based strategies—are opening up fresh avenues for deeper, lasting healing. Could these breakthroughs hint at a potential permanent solution? Let’s explore how cutting-edge findings, combined with innovative functional medicine techniques, are paving the way for a brighter future in psoriasis care!
Psoriasis is More Than Just Skin Deep Issue
While Psoriasis might first appear to be just a skin condition, it runs much deeper than that. It’s a systemic autoimmune disease characterised by red, scaly patches and ongoing inflammation resulting from an overactive immune system that is attacking and damaging the skin. But psoriasis is not just about the skin; it is associated with other underlying health issues and can also lead to some, including:
- Elevated Cardiovascular Risks: This chronic inflammation linked to psoriasis entails an increased risk of heart conditions, stroke, and other cardiovascular conditions.
- Mental Health Challenges: Many experience depression, anxiety, and social isolation because of the visible symptoms and stigma.
- Metabolic Syndrome Link: Psoriasis is strongly linked to obesity, high blood pressure, and insulin resistance, amplifying health complications.
- Gut dysbiosis: Imbalance of gut bacteria disturbs the immune system, raises inflammation, and triggers psoriasis flares by damaging digestion and nutrient absorption.
- Slow liver: An inefficient liver is unable to detoxify the body, and toxins accumulate, which worsens inflammation and skin diseases such as psoriasis.
- Nutrient deficiencies: Inadequate amounts of critical vitamins (D, A, E) and minerals (zinc, magnesium) compromise skin healing, retard immune function, and enhance the severity of psoriasis symptoms.
- Overgrowth of Candida: Yeast overgrowth in the gut interferes with microbiome balance, compromises gut lining integrity, and initiates systemic inflammation, exacerbating autoimmune diseases such as psoriasis.
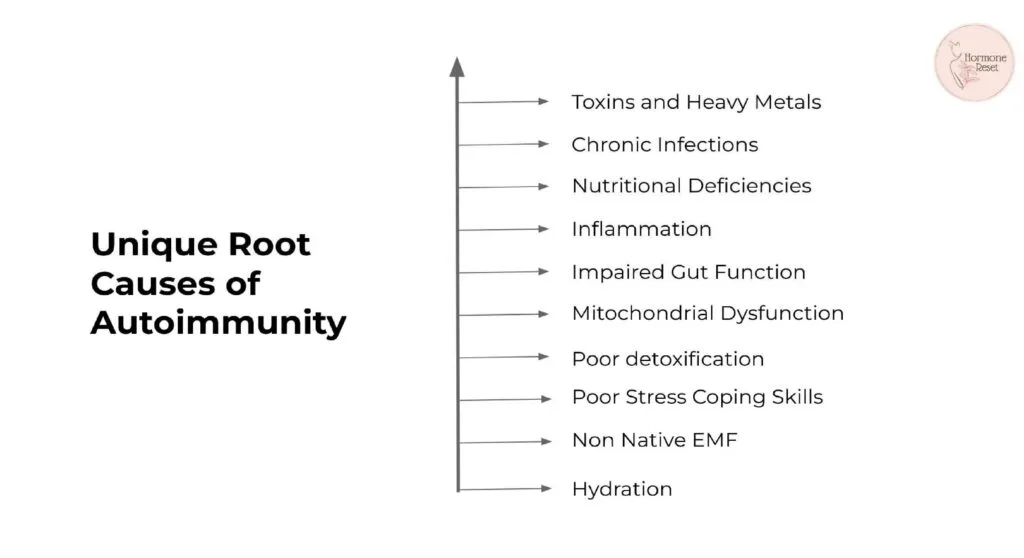
Recognizing these deeper connections is crucial for addressing the root causes of psoriasis rather than just its visible manifestations.
Conventional Treatments are just a Band-Aid for a Chronic Condition
For decades, psoriasis treatment has focused on symptom management through therapies like corticosteroids, biologics, and phototherapy. While effective to some extent, these methods leave significant gaps:
- Short-Lived Relief: Symptom suppression often leads to recurring flare-ups without addressing the underlying causes.
- Side Effects and Risks: The prolonged use of certain drugs can cause various side effects like liver damage, immune suppression, dependency etc.
- Cost-Prohibitive: Advanced biologic treatments, even if effective, remain costly and inaccessible for many patients.
The future of psoriasis care demands a shift toward personalized, integrative approaches that prioritize root cause resolution over symptom suppression.
Also Read: Living With Multiple Autoimmune Conditions
Hormone Reset is A Revolutionary Path to Healing Psoriasis
The Hormone Reset approach offers a thoughtful and holistic method to address the interconnected systems of your body, promoting long-lasting healing. Rather than relying on conventional treatments, this strategy focuses on identifying the root causes leading to immune dysfunction, gently rebalancing your hormones, reducing inflammation, and tackling systemic issues right at their source.
The Role of Hormones in Psoriasis
Hormones such as cortisol, insulin, and thyroid hormones are incredibly important for managing our immune system and inflammation. When these hormones are out of balance, it can make psoriasis symptoms worse. Let’s explore how bringing them back into balance can make a positive difference:
- Managing Cortisol for Reduction of Stress: Chronic stress elevates cortisol, which initiates immune dysfunction. Yogic techniques and mindfulness can reduce cortisol levels, as can adaptogenic herbs like ashwagandha and Rhodiola.
- Enhances insulin sensitivity: Insulin resistance is a key factor source of systemic inflammation. Dietary improvement that thrives on low-glycemic foods, whole grains, lean proteins, and healthy fats can improve one’s insulin sensitivity significantly.
- Thyroid Health for Skin Wellness: Many people with psoriasis have hypothyroidism. Other nutrients that really can be important for thyroid health include selenium (Brazil nuts) and iodine (seaweed).
What is the connection of Psoriasis and Gut Issue?
Emerging research highlights the powerful link between gut health and skin conditions like psoriasis. An imbalanced gut microbiome or leaky gut syndrome can worsen inflammation and immune responses.
- Eliminating Dietary Triggers: Gluten, dairy, and processed foods are common culprits that exacerbate gut inflammation.
- Prioritising Probiotic Foods: Fermented foods like yoghurt, kimchi, and kefir restore gut microbial balance. However, it is important to note that gut infections can be worsened by probiotic foods. Hence, cleaning up infections is important before introducing probiotic-rich foods. In such cases, specific probiotic supplements are a better alternative.
- Essential Nutrients Boost: Zinc, omega-3 fatty acids, and vitamin D all enhance gut health and decrease systemic inflammation.
Also Read: Understanding The Connection Between Your Diet And Hormonal Imbalance
Detoxification: Clearing Out the Toxins
The liver is vital for hormone metabolism and toxin elimination. A sluggish liver can lead to a buildup of inflammatory substances, and worsening psoriasis.
- Liver-Supporting Foods: Cruciferous vegetables (broccoli, kale), citrus fruits, and garlic enhance detoxification.
- Herbal Allies: Milk thistle and dandelion root will help support liver function.
- Sweat Therapy: Infrared saunas, regular exercise, and Epsom salt baths help detoxify the skin and body.
Calming the Fire Within
Chronic inflammation is at the heart of psoriasis. Tackling it holistically can bring profound relief:
- Anti-Inflammatory Diet: Turmeric, ginger, green tea, and fatty fish are some of the inflammation-fighting foods.
- Identify Environmental Triggers: Mold exposure, harsh chemicals, and allergens make symptoms worse.
- Reducing toxin exposure: Replace toxic personal care products and chemical-based household cleaners to reduce inflammatory burden.
Scientific Breakthroughs in Psoriasis Care
Recent studies are shedding light on the effectiveness of integrative approaches. Key findings include:
- Hormonal Balance Yields Amazing Results: A 2023 PMC study showed that patients who used hormone reset strategies experienced fewer flare-ups and less severe symptoms.
- Gut Healing Improves Outcomes: Probiotic and prebiotic supplementation strengthened gut barriers and reduced systemic inflammation in clinical trials.
- Detox protocol success: Improvements in dermal health along with better symptomatic control are noted for those detox-focused interventions.
Are there any Future Innovations for Permanent Cure For Psoriasis?
Microbiome-Focused Therapies: Targeting specific probiotic strains holds immense promise for reducing psoriasis severity by restoring gut health.
Precision Nutrition and Nutrigenomics: Customized diets based on genetic profiles can suppress inflammatory pathways linked to psoriasis.
Epigenetic Modifications: Lifestyle changes like improved sleep, regular exercise, and reduced stress can reprogram gene expression and reduce psoriasis symptoms.
AI-Powered Care: Artificial intelligence is revolutionizing personalised medicine, offering tailored treatment plans based on an individual’s unique biology and lifestyle
How to Treat Psoriasis?
Ready to embrace the Hormone Reset approach for Permanent Cure For Psoriasis? Here’s how you can begin:
- Adopt a Psoriasis-Friendly Diet
- Focus on whole, nutrient-dense foods like leafy greens, lean proteins, and healthy fats.
- Avoid inflammatory triggers such as sugar, processed foods, and gluten.
- Prioritise Stress Management
- Incorporate daily mindfulness practices or yoga sessions.
- Try natural adaptogens like holy basil and ashwagandha to lower cortisol levels.
- Strengthen Your Gut
- Add probiotic-rich foods and supplements to your routine.
- Include prebiotic-rich foods like garlic, spring onions, and millet for microbial balance.
- Support Detoxification
- Start your day with warm lemon water to stimulate liver function.
- Use herbal teas like dandelion and turmeric for natural detox benefits.
- Seek Expert Guidance
- Consult a functional medicine practitioner for a tailored plan.
- Explore resources like Hormone Reset for specialized support
If you’re looking for a complete Recipes, then checkout our Recipes for managing your Psoriasis
Reimagining Psoriasis with A Hopeful Tomorrow
A definitive Permanent Cure For Psoriasis is available with the Hormone Reset approach, which stands out as a guiding light. By focusing on the underlying causes, such as hormonal imbalances, gut health concerns, and chronic inflammation, this functional medicine method can offer people lasting remission and a better quality of life.
Picture waking up to clear skin, feeling vibrant and full of energy, and exuding newfound confidence. Healing starts with understanding your body’s needs and embracing positive, evidence-based changes. The future of psoriasis treatment is here—are you ready to embrace it?
Further if you’re looking for one-on-one consultation with our expert then Book Now!
References
- Ahlehoff O, Gislason GH, Charlot M, Jorgensen CH, Lindhardsen J, Olesen JB, Abildstrom SZ, Skov L, Torp-Pedersen C, Hansen PR 2011. Psoriasis is associated with clinically significant cardiovascular risk: A Danish nationwide cohort study. J Intern Med 270: 147–157
- Arican O, Aral M, Sasmaz S, Ciragil P 2005. Serum levels of TNF-α, IFN-γ, IL-6, IL-8, IL-12, IL-17, and IL-18 in patients with active psoriasis and correlation with disease severity. Mediators Inflamm 2005: 273–279
- van de Kerkhof PCM, Nestle FO 2012. Psoriasis. In Dermatology (ed. Bolognia JL, Jorizzo JL, Schaffer JV). Elsevier, Amsterdam
- Tarkin JM, Rudd JH. Psoriasis: More Than Just Skin Deep. Arterioscler Thromb Vasc Biol. 2015 Dec;35(12):2487-8. doi: 10.1161/ATVBAHA.115.306560. PMID: 26607356; PMCID: PMC4704140.
- Blackstone B, Patel R, Bewley A. Assessing and Improving Psychological Well-Being in Psoriasis: Considerations for the Clinician. Psoriasis (Auckl). 2022 Mar 25;12:25-33. doi: 10.2147/PTT.S328447. PMID: 35371967; PMCID: PMC8965012.
- Hao Y, Zhu YJ, Zou S, Zhou P, Hu YW, Zhao QX, Gu LN, Zhang HZ, Wang Z, Li J. Metabolic Syndrome and Psoriasis: Mechanisms and Future Directions. Front Immunol. 2021 Jul 23;12:711060. doi: 10.3389/fimmu.2021.711060. PMID: 34367173; PMCID: PMC8343100.
- Boehncke WH. Systemic Inflammation and Cardiovascular Comorbidity in Psoriasis Patients: Causes and Consequences. Front Immunol. 2018 Apr 5;9:579. doi: 10.3389/fimmu.2018.00579. PMID: 29675020; PMCID: PMC5895645.
- Chen L, Li J, Zhu W, Kuang Y, Liu T, Zhang W, Chen X, Peng C. Skin and Gut Microbiome in Psoriasis: Gaining Insight Into the Pathophysiology of It and Finding Novel Therapeutic Strategies. Front Microbiol. 2020 Dec 15;11:589726. doi: 10.3389/fmicb.2020.589726. PMID: 33384669; PMCID: PMC7769758.
- Barrea L, Savanelli MC, Di Somma C, Napolitano M, Megna M, Colao A, Savastano S. Vitamin D and its role in psoriasis: An overview of the dermatologist and nutritionist. Rev Endocr Metab Disord. 2017 Jun;18(2):195-205. doi: 10.1007/s11154-017-9411-6. PMID: 28176237; PMCID: PMC5486909.
Share