Table of Contents
Introduction
Have you ever felt “butterflies” in your stomach before a big event? Or experienced digestive discomfort during stressful times? These experiences are not random — they are signs of the powerful connection between your gut and brain.
The gut–brain axis (GBA) is a complex, two-way communication system that links your digestive system and your brain. When this connection is healthy, you feel emotionally balanced, mentally clear, and physically well. When it becomes disrupted, it can contribute to chronic inflammation, mood disorders, digestive problems, and autoimmune conditions.
Understanding this connection allows us to address many chronic health issues at their root.
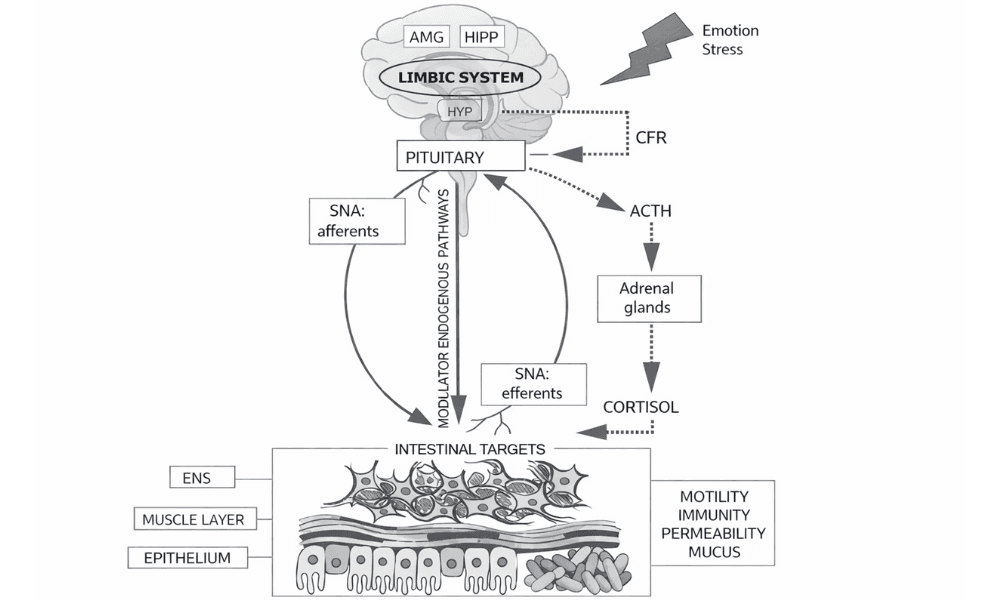
What Is the Gut–Brain Axis?
The gut–brain axis is a bidirectional communication network involving:
- The Central Nervous System (CNS)
- The Autonomic Nervous System (ANS)
- The Enteric Nervous System (ENS) — often called the “second brain”
- The Hypothalamic–Pituitary–Adrenal (HPA) axis
This system connects emotional and cognitive centers of the brain with intestinal functions such as:
- Gut motility
- Immune activation
- Intestinal permeability
- Hormone release
- Stress response
Communication occurs through nerves (especially the vagus nerve), hormones, immune messengers, and microbial metabolites.
In simple terms: Your gut influences your nervous system and vice versa.

Conditions Linked to Gut–Brain Axis Dysfunction
When the gut–brain communication is disrupted, it can contribute to multiple chronic conditions:
Mental Health
- Anxiety
- Depression
- ADHD
- Autism spectrum disorders
Neurological Disorders
- Alzheimer’s disease
- Parkinson’s disease
- Migraines
Digestive Conditions
Autoimmune Disorders
- Hashimoto’s thyroiditis
- Multiple sclerosis
- Rheumatoid arthritis
These conditions often share underlying factors: chronic stress, inflammation, and microbiome imbalance.
The Role of Gut Microbiota
Your gut contains trillions of microorganisms that directly influence your brain and immune system.
1. Neurotransmitter Production
About 95% of serotonin is produced in the gut. Gut bacteria also influence GABA and dopamine production — essential for mood regulation, sleep, focus, and stress resilience.
2. Immune Regulation
Approximately 70% of the immune system resides in the gut. In the gut there are tight junctions.These junctions make the intestinal barrier impermeable to toxins and other materials. If the intestinal barrier becomes permeable (“leaky gut”), toxins and inflammatory compounds enter the bloodstream, triggering systemic and even brain inflammation.
3. Short-Chain Fatty Acids (SCFAs)
Beneficial bacteria ferment dietary fiber to produce SCFAs like butyrate, which:
- Strengthen the gut lining
- Reduce inflammation
- Support brain function
- Regulate immune balance
4. Stress Response
Chronic stress activates the HPA axis, increasing cortisol levels. High cortisol disrupts the gut barrier, alters microbiome balance, and weakens vagus nerve signaling.

How to Restore the Gut–Brain Axis Naturally?
Healing the gut–brain axis requires a holistic approach. Below is a detailed, step-by-step strategy.
1. Remove Inflammatory Triggers
The first step is reducing the burden on the gut.
Eliminate Common Irritants:
- Refined sugar
- Ultra-processed foods
- Excess alcohol
- Artificial additives
- Gluten or dairy (if sensitive)
Identify Hidden Causes:
- Small Intestine bacterial overgrowth
- Candida overgrowth
- Parasites
- Food intolerances
Removing these triggers reduces inflammation and allows the gut lining to begin repairing itself.
2. Rebuild and Diversify the Microbiome
A diverse microbiome is essential for strong gut–brain communication.
Increase Fiber Intake
Aim for a variety of plant fibers:
- Leafy greens
- Vegetables
- Fruits
- Legumes
- Seeds
- Resistant starch (green bananas, cooked and cooled rice or potatoes)
Fiber feeds beneficial bacteria, increasing SCFA production.
Use Targeted Probiotics (If Needed)
Strains like Lactobacillus and Bifidobacterium are associated with improved mood and reduced inflammation.
3. Repair the Gut Lining
If intestinal permeability is present, focus on strengthening the barrier.
Key Nutrients:
- L-glutamine (supports intestinal cells)
- Zinc (tight junction support)
- Omega-3 fatty acids (reduce inflammation)
- Collagen or bone broth (supports tissue repair)
- Aloe vera (soothing and anti-inflammatory)
A healthy gut lining prevents toxins from entering the bloodstream and triggering brain inflammation.
4. Regulate Stress & Support the HPA Axis
Chronic stress is one of the biggest disruptors of the gut–brain axis.
Daily Stress Regulation Practices:
- Deep diaphragmatic breathing (5–10 minutes daily)
- Meditation or mindfulness
- Gentle yoga
- Nature exposure
- Journaling
These practices lower cortisol levels and improve gut motility and microbiome balance.
5. Strengthen the Vagus Nerve
The vagus nerve is the main communication highway between the gut and brain.
Natural Vagus Nerve Stimulation:
- Slow, controlled breathing
- Humming or chanting
- Singing
- Gargling
- Cold water exposure
- Regular social connection
Improved vagal tone enhances digestion, reduces inflammation, and stabilizes mood.
6. Optimize Sleep
Sleep is critical for gut repair and neurotransmitter balance.
Improve Sleep Quality:
- Maintain consistent sleep schedule
- Reduce screen exposure before bed
- Keep bedroom cool and dark
- Avoid heavy meals late at night
Sleep deprivation disrupts gut bacteria and increases inflammatory markers.
7. Anti-Inflammatory Diet for Brain Support
Adopt a whole-food, nutrient-dense diet:
- Healthy fats (olive oil, nuts, seeds, fatty fish)
- Colorful vegetables
- High-quality protein
- Herbs and spices like turmeric and ginger
Avoid chronic blood sugar spikes, as glucose instability worsens inflammation and mood instability.
8. Support Neurotransmitter Balance Naturally
Rather than immediately relying on medications, support the body’s natural production:
- Tryptophan-rich foods (pumpkin seeds, turkey, eggs)
- Magnesium for relaxation
- Adaptogens like ashwagandha and rhodiola (if appropriate)
Always consult a healthcare provider before supplementation.
Frequently Asked Questions
1. What is the gut–brain axis, and why is it important?
The gut–brain axis is the communication network that connects the digestive system and the brain through nerves, hormones, immune signals, and the gut microbiome. This two-way communication allows the brain to influence digestive processes while the gut can affect mood, cognition, and overall health. A well-functioning gut–brain axis supports emotional balance, healthy digestion, immune strength, and mental clarity.
2. Can gut health affect mental health?
Yes, gut health plays a significant role in mental health. The gut microbiome influences the production of neurotransmitters such as serotonin, dopamine, and GABA, which regulate mood, sleep, and stress responses. Since a large portion of serotonin is produced in the gut, imbalances in gut bacteria can contribute to anxiety, depression, and other mood disorders.
3. What are the signs of an unhealthy gut–brain connection?
An imbalance in the gut–brain axis can lead to a variety of symptoms affecting both physical and mental health. Common signs include digestive problems such as bloating, constipation, or irritable bowel syndrome, as well as symptoms like brain fog, fatigue, sleep disturbances, mood swings, and increased stress sensitivity. These symptoms often indicate inflammation, microbiome imbalance, or increased intestinal permeability.
4. How can you improve the gut–brain axis naturally?
Improving the gut–brain axis requires a holistic approach that focuses on diet, lifestyle, and stress management. Eating a nutrient-dense diet rich in fiber, vegetables, and fermented foods helps nourish beneficial gut bacteria. Managing stress through meditation, breathing exercises, or physical activity can regulate the stress response system. Getting adequate sleep, reducing processed foods and sugar, and maintaining a balanced lifestyle can also help restore healthy communication between the gut and brain.
5. How long does it take to restore gut–brain balance?
The time needed to improve the gut–brain axis varies depending on the individual and the underlying health issues involved. Some people may notice improvements in digestion, mood, and energy levels within a few weeks after adopting healthier habits. However, restoring microbiome balance and reducing chronic inflammation can take several months of consistent dietary changes, stress management, and lifestyle adjustments.
Conclusion
The gut–brain axis is not just a theory — it is a foundational system that influences mental clarity, emotional balance, immune function, and chronic disease risk.
By removing inflammatory triggers, rebuilding the microbiome, repairing the gut lining, regulating stress, and supporting the vagus nerve, you can naturally restore this powerful communication pathway.
Healing the gut is not just about digestion — it is about restoring balance to the entire body and mind.
When the gut is supported, the brain begins to heal — and true wellness becomes possible.

References
- The gut-brain axis: interactions between enteric microbiota, central and enteric nervous systems– National Library of Medicine
- Gut feelings: The Emerging Biology of Gut–Brain Communication–Springer Nature Limited
- Minireview: Gut Microbiota: The Neglected Endocrine Organ– Molecular Endocrinology
- Gut–brain axis: how the microbiome influences anxiety and depression– Science Direct
- Mind-altering microorganisms: the impact of the gut microbiota on brain and behaviour– Springer Nature Limited
Please subscribe to our social channels for updates related to functional medicines.
Instagram: thehormonereset
Facebook: Hormone Reset
YouTube: Hormone Reset Program
LinkedIn: Hormone Reset





Leave a Reply